Deep Vein Thrombosis
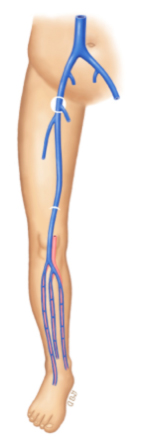
What is deep vein thrombosis? — Deep vein thrombosis is the medical term for blood clots in the deep veins of the leg. Deep vein thrombosis, or “DVT” for short, can be dangerous.
If a blood clot forms inside a blood vessel, it can clog the vessel and keep blood from getting where it needs to go. When that happens to one of the veins deep within the leg, blood can back up and cause swelling and pain.
Another problem with blood clots in veins is that they can travel to other parts of the body and clog blood vessels there. Blood clots that form in the legs, for example, can end up blocking blood vessels in the lungs. This can make it hard to breathe and sometimes, when they are large, can lead to death. When blood clots travel to the lungs surgeons call it “pulmonary embolism” or “PE.”
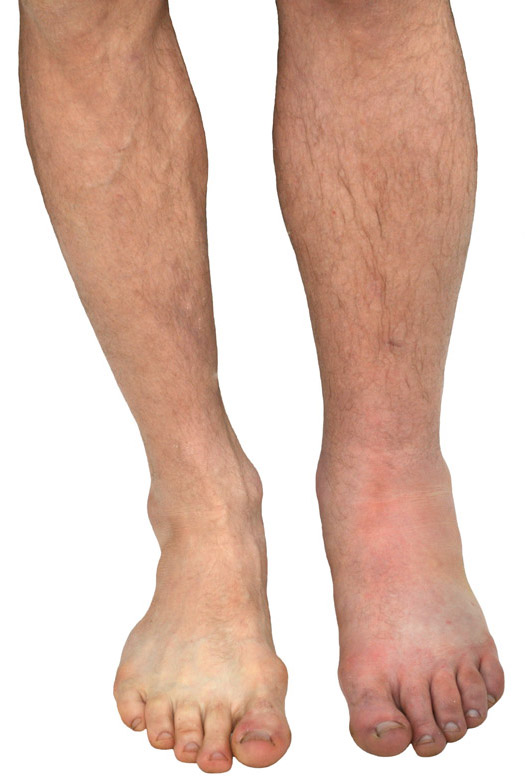
What are the symptoms of DVT? — DVT can cause:
- Swelling
- Pain
- Warmth and redness in the involved leg
Sometimes clots form in the veins that are closer to the surface of the skin, called the superficial veins. Those blood clots cause a different set of symptoms. Blood clots in the veins near the surface of the skin are more painful and cause redness or infection. These clots sometimes also cause the veins to harden and bulge into ridges that look like cords. This is most common with the veins below the knee.
If you think you have a blood clot in your leg, call your doctor right away. Blood clots in the veins near the surface of the skin are less dangerous. But blood clots in the deep veins of the leg are more serious. Your doctor can refer to you to VVC for tests to find out if you do have a clot that needs to be treated.
What are the symptoms of blood clots in the lungs? — Blood clots in the lungs can cause:
- Panting, shortness of breath, or trouble breathing
- Sharp, knife-like chest pain when you breathe in or strain
- Coughing or coughing up blood
- A rapid heartbeat
If you get any of these symptoms, especially if they happen over a short period of time call 000 immediately.
How is DVT treated? — DVT is treated with medicines that keep the clot from getting bigger and travelling to the lung. Some of these medicines come in shots and others come in pills.
People who have had clots are usually put on medicines to prevent future blood clots, called blood thinners. Almost everyone is put on a blood thinner that comes in a pill for at least 3 months (and usually longer). Some people are put on a medicine that is injected under the skin called heparin. This might be for a few days, or longer if for some reason they can’t take pills.
Blood thinners do not dissolve existing blood clots but they do keep them from getting bigger. They also help keep new blood clots from forming. Being on a blood thinner for a few months is important because it gives the body time to dissolve the old clot. It’s also important because people who have a clot are at risk of developing another clot, especially in the first few months.
There are a few different blood thinner medicines. One of the most commonly used medicines is warfarin but other options exist. If your doctor puts you on a blood thinner, take it exactly as directed. If you forget or miss a dose, call your doctor to find out what to do. When you start taking a blood thinner, you will need to have your blood tested. If you are treated with warfarin, the effects can change over time, so your blood will need to be checked frequently. If there are changes, your doctor might need to adjust your dose. At the wrong doses, the drug can either stop working or lead to serious bleeding. In fact, bleeding is a risk with all the blood thinners, so you and your doctor should also always watch out for sign of bleeding.
Can I do anything on my own to prevent blood clots? — Yes. People sometimes form clots because they have been sitting still for too long. People who travel on long airplane flights, for example, are at increased risk of blood clots. Here are some things you can do to help prevent a clot during a long flight:
- Stand up and walk around every 1 to 2 hours
- Do not smoke just before your trip
- Wear loose, comfortable clothes
- Shift your position while seated, and move your legs and feet often
- Drink plenty of fluids
- Wear knee-high compression stockings
- Avoid alcohol and medicines that make you sleepy, because they can impair your ability to move around